How 3-D Printing is Changing Surgical Care at Duke
Custom-made models help doctors plan and practice surgeries before entering the operating room.
Duke’s 3-D printing services can convert medical scans into personalized models of bones, organs and other tissues. Video by Wil Weldon at http://wilweldon.com/.
DURHAM, N.C. -- Earlier this year, a 21-year-old woman went to Duke Orthopedics with a painful hip. She had a hip deformity that made it difficult to walk without limping. To figure out the best treatment, her doctors turned to an unusual tool: 3-D printing.
The technique uses a digital image -- in this case MRI and CT scans of the patient’s pelvis -- to create an exact 3-D replica of the patient’s anatomy.
The doctors began by sending the patient’s scans to specialists in the Duke Multi-Dimensional Imaging Lab, who digitally isolated the hip joint and converted it to a file that 3-D printers can read.
The printable file was then sent to the 2,000-square-foot Co-Lab Studio on West Campus, where more than 60 3-D printers deposit tiny droplets of plastic “ink” in successive layers that harden to make 3-D shapes.
These custom-made models are helping Duke doctors and medical researchers plan and practice surgeries before entering the operating room.
As the patient was in her early 20s, an operation to salvage and reconstruct the damaged hip joint seemed the best option at first. But the 3-D printed model changed their minds. It showed she had wear and tear on her cartilage that was allowing her bones to rub together. She needed a hip replacement instead.
“The best thing we can do for our patients is think before we cut,” said Robert Kollmorgen, M.D., a 2016-2017 hip preservation fellow under the guidance of orthopedic surgeon Steven Olson, M.D., at Duke Health.
“The 3-D printed model allowed us to be better planners up front and map out what we feel is the best surgery we could offer her,” Kollmorgen said.
The case was the first time 3-D printing technology had been used in more than 200 hip surgeries at Duke so far this year. But Kollmorgen says the life-sized model helped doctors understand the patient’s unique anatomy better than they could by relying solely on MRI or CT scans viewed on a flat screen.
As a result Olson and Kollmorgen were able to plan her surgery with millimeter precision, including where to make cuts or place implants, with less adjustment time in the operating room.
Worldwide, 3-D printing has been used in medicine since the early 2000s. The technology was first used to make dental crowns and dentures, custom-fit prosthetic limbs, hearing aids with tailor-made ear buds and other rigid devices where standard sizes often don’t fit.
Researchers at Duke and elsewhere have since 3-D printed models of breasts, hearts, knee menisci, ears and other soft tissues, some made to mimic the feel of the real thing.
 General surgery resident Alice Wang, M.D., and cardiologist Sreekanth Vemulapalli, M.D., are using 3-D printing to model the flexible anatomy of the aorta in the hopes of avoiding potential complications from a popular heart procedure.
General surgery resident Alice Wang, M.D., and cardiologist Sreekanth Vemulapalli, M.D., are using 3-D printing to model the flexible anatomy of the aorta in the hopes of avoiding potential complications from a popular heart procedure.
Many of their patients suffer from a disease called aortic stenosis, where the heart’s aortic valve stiffens over time and no longer opens all the way. Often caused by calcium buildup, the narrowing of the valve slowly constricts blood flow from the heart to the rest of the body.
Tens of thousands of Americans over 65 are hospitalized each year for the condition, which causes shortness of breath, chest pain, fatigue and fainting.
For years the standard treatment has been to replace the valve with open heart surgery. But a newer procedure called transcatheter aortic valve replacement, or TAVR, uses a catheter to replace the heart valve instead of opening the chest and removing the old one.
 The new valve is folded up, slipped into a small tube -- usually through a blood vessel in the leg -- then threaded up to the heart where it is opened like an umbrella, pushing aside the old valve and wedging the new one in its place.
The new valve is folded up, slipped into a small tube -- usually through a blood vessel in the leg -- then threaded up to the heart where it is opened like an umbrella, pushing aside the old valve and wedging the new one in its place.
Because there isno big incision, heart valve replacement with TAVR offers a less invasive alternative and shorter recovery time for patients who are too frail or sick to undergo open-heart surgery. But the procedure has its limits.
Without direct access to the patient’s heart, Wang says, the complex anatomy of the aorta where it attaches to the heart and the irregular pattern of calcium deposits on the valve can make it difficult to predict how the new valve will fit once it’s in place. The result is that sometimes the new valves leak slightly around the edges.
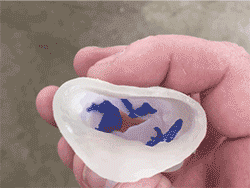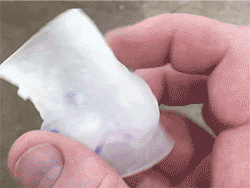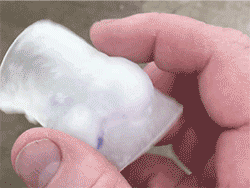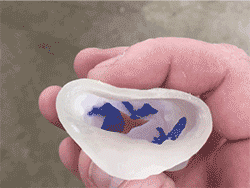
Wang realized 3-D models might be able to help test fit replacement valves and identify potential leaks before they happen. She collaborated with the Co-Lab Studio’s 3-D printing team to make replicas of damaged aortic valves from CT scans of 10 patients.
Soft tissues were printed using a flexible material; the calcium deposits using a more rigid material.
As a first step, Wang fitted the 3-D-printed models with standard replacement valves and shined light through them to predict which patients were likely to develop leaks.
The goal, Wang says, is to help doctors better visualize how a new valve will fit inside a patient’s heart and where to place it to ensure a proper seal.
“This really allows us to guide our treatment for each individual patient and personalize their experience,” Wang said.